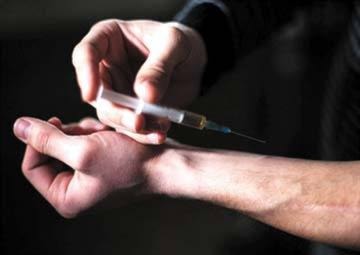
Barry Coulter
An increase in overdose deaths is accompanying an increase in availability and type of illicit drugs in southeast B.C.
According to Interior Health and ANKORS (Aids Network Outreach & Support Society) recent BC Coroner statistics show there has been a gradual increase in opioid related overdose deaths over the last 24 months across B.C., including communities within Interior Health. In addition, community agencies continue to receive reports about individuals experiencing fatal and non-fatal overdoses.
Dr. Trevor Corneil, Medical Health Officer for Interior Health said that with a general increase in the number of overdose deaths, related to illicit drugs, more than 80 per cent of them have an opioid involved or detected post mortem. The majority of overdose symptoms are being reported after using opioid drugs such as OxyContin and heroin.
“The availability of drugs on the illicit market has been increasing,” Dr. Corneil said in an interview with the Townsman. “The number of options and types of drugs within that market have been increasing, and we don’t have a lot of control over that.”
Dr. Corneil said it is important to know there is not one particular group being affected.
“We have those people with significant mental health issues and significant addiction problems who are dying, but we also have recreational users. People don’t realize that there are recreational injection drug users. Those people are at risk as well.”
Every year, at least since 2008, has shown a gradual but steady increase in the number of overdose deaths.
“In Interior Health in 2008, there 20 overdose deaths related to illicit drugs, and in 2015 there were 60,” Dr. Corneil said. “So every year it was more than the year before — basically a straight line heading up.
“Into this year, we already have some preliminary numbers from January — they’re preliminary because the data is fluid in the sense that coroners are constantly adjusting or changing decisions that are made around the final cause of death. But the preliminary number for January is 15 overdose deaths for the region. It’s a trend, unless the February total was nine. I wouldn’t call it a spike yet, until we have a couple more months of data.”
‘A Market Clearly
Having Some Success’
Information coming forward shows there is not one specific “bad batch” of drugs. The majority of overdose symptoms are being reported after using opioid drugs such as OxyContin and heroin.
“What’s interesting is that we’re seeing it everywhere. Certainly the bigger cities are being impacted, but so are the smaller cities. Where this was really a ‘never occurrence’ in the Cranbrook/Trail area, we’ve see anywhere between one and three every year for the past three years, and that is likely to increase.”
There has been a lot of recent publicity concerning the painkiller fentanyl, which has become a problem in terms of substance abuse. But Dr. Corneil says Fentanyl is “only one piece of the puzzle.”
“We have seen an increase in fentanyl — fentanyl has flooded the market in the last five years. About a third of cases have fentanyl detected in the system post-mortem. But two thirds of the cases are not fentanyl related. If you pulled out all those cases, you would still see increasing trends that speaks to access and a market (market for illicit drugs) clearly … having some success.
“Heroin is the same drug it always was. The problem is that like fentanyl it’s an opiate, and opiates suppress the respiratory system in a very uncontrollable way. You have to be really knowledgeable as a user if you’re going to try and use it safely, or at least in a safer way. That’s why we speak a lot about education and knowledge awareness, testing, using smaller doses or hits before your usual amount so you know what you’re using.”
Interior Health has several harm reduction programs to help users, including a Take Home Naloxone program that trains participants to recognize and respond to an overdose situation, using a naloxone kit. Naloxone can reverse (stop) an opioid overdose – in the event of an overdose, naloxone restores breathing within 2-5 minutes of administration and offers the opportunity to save a life and reduce harm related to the overdose while waiting for help to arrive.
“And of course access to treatment is essential, these are opportunities to get people into treatment when they’re ready, and I think that’s the direction we need to go,” Dr. Corneil said.
‘Safe Injection Sites In Our Future’
The subject of safe injection sites, as exist in Vancouver, is likely to become a subject of discussion across the province, and perhaps a reality, Dr. Corneil said.
“There’s been a lot of questions about safe consumption sites, or safe injection sites as they’re also known,” he said. “They’ve been shown to be very effective for a specific population — those who are heavy users or those who are brand new to using, particularly the injection route. In British Columbia we know the Appeals Court in B.C., also the Supreme Court of Canada ruled that these are in fact health care sites and therefore can be exempted under Section 56 of the Controlled Substances And Drugs Act.”
The federal government in fact has recently given approval for a second safe injection site in Vancouver.
“Certainly indication are that the current government is showing interest in evidence and acknowledging that these do work,” Dr. Corneil said. “It has begun to open up the discussion for these as options for people.
“Will we see one in Interior Health? Very possibly in the next year or two. We’re looking at feasibility right now, whether stakeholders are interested, and once we have a proposal that makes some kind of sense we’ll be able to bring that to the community and engage stakeholders and community members in that discussion.”
Interior Health and its partners like ANKORS offer a variety of programs including: withdrawal management, opioid replacement therapy, counselling, and housing supports. To access treatment services, talk to your physician or contact one of the agencies listed below.
Interior Health Mental Health and Substance Use Services
Cranbrook: 250- 342-3868
Trail: 250-364-6262
Nelson: 250-505-7248
ANKORS: 1-800-421-2437